If you’ve ever sat across from a stack of unprocessed claims at the end of a long clinic day, you already know the problem. Medical billing isn’t just paperwork. It’s the financial engine of your entire practice. When it runs smoothly, everything else can too. When it doesn’t, the ripple effects reach far beyond the billing department.
Industry estimates suggest that healthcare providers lose 5% to 10% of potential billing revenue due to inefficiencies, undercoding, delayed submissions, and denials that go unappealed for a mid-sized practice, which can translate to hundreds of thousands of dollars left on the table every single year. And yet, billing rarely gets the strategic attention it deserves, because most providers are busy doing what they trained to do: delivering care.
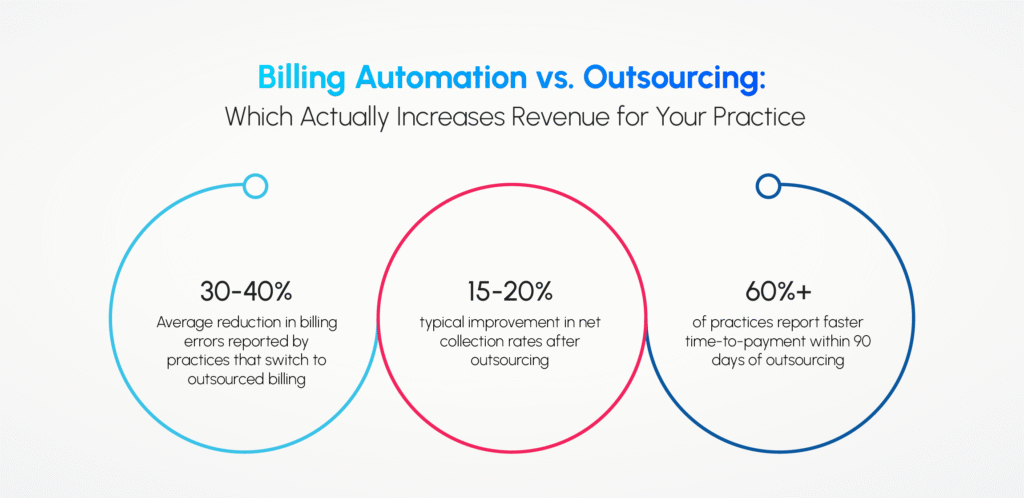
Healthcare providers today are broadly choosing between two approaches billing automation vs. outsourcing to make their billing more efficient. The first is automation software, and the second is outsourcing to a third-party service. Both promise to reduce errors and recover more revenue. But they work very differently and for different types of practices, one may suit far better than the other
Let’s break billing automation vs. outsourcing down honestly, so you can see the full picture before making any decisions.
The Case for Billing Automation
Billing automation refers to software platforms and tools that handle repetitive billing tasks such as eligibility verification, claim scrubbing, coding suggestions, payment posting, and follow-up reminders with minimal human intervention.
The appeal is easy to understand. Modern practice management systems and revenue cycle management (RCM) software can process claims faster than any human team, catch common errors before submission, and generate detailed reports that give you a real-time view of your financial health.
Where automation genuinely excels
- Speed at scale
Automated systems can verify patient eligibility in seconds something that might take a billing coordinator several minutes per patient. Across a busy practice, that adds up to hours saved every week.
- Consistency
Software doesn’t have bad days. It applies the same rules every time, which means fewer human errors in code entry or claim formatting.
- Real-time visibility
Dashboards let you see your accounts receivable aging, denial rates, and collection trends without waiting for a weekly report.
- Data ownership
Everything stays in your system. You control your patient data and financial records at all times.
That said, automation is only as good as the people operating it. The software doesn’t negotiate with a payer on a denied claim, and it doesn’t recognize that a specific insurance plan in your region may have quirks in how it processes certain codes. Human expertise still matters, automation simply reduces how much repetitive work humans need to do
The honest challenges of automation
Implementing billing software comes with a learning curve and often a high upfront cost. Your in-house staff needs to be trained, and they need time to become proficient. During that transition period, billing can slow down, and errors can actually increase temporarily.
Smaller practices, especially, may find that the full ROI of a sophisticated RCM system takes 12 to 18 months to materialize. And if your team doesn’t use the system to its full potential, you’re paying for capabilities you never actually use.
There’s also the question of ongoing maintenance. Payer rules, coding requirements, and compliance regulations change frequently. While software platforms update their systems, it’s still on your staff to stay current to understand when a system update changes a workflow, or when a new payer policy means your automated rules need adjusting.
For practices without a dedicated billing manager, this ongoing upkeep is often underestimated when evaluating the true cost of an in-house automation solution
The Case for Outsourcing Medical Billing
Outsourcing means handing off your billing operations, or specific parts of them, to a dedicated external billing company. These companies employ certified medical coders and billing specialists whose entire job is to maximize your revenue cycle performance.
For many practices, this is the more transformative choice. Here’s why.
What outsourcing actually delivers
When you work with a professional billing service, you’re not just getting software, you’re getting a team. That team brings deep payer-specific knowledge, denial management expertise, and compliance awareness that would take years to build in-house.
Good outsourced medical billing companies also invest heavily in staying current. When regulations change or payers revise how they process certain codes, their teams adapt immediately because billing is their core business.
One of the most underappreciated advantages of outsourcing is what it does for your staff’s bandwidth. When your front desk and clinical coordinators aren’t chasing claims or decoding EOBs, they can focus on patient experience, scheduling efficiency, and care coordination the things that actually grow your practice long-term
The concerns providers typically have
Q1: Will I lose control if I outsource my billing?
No. A good billing partner provides transparent reporting, giving you full visibility into every claim, payment, and denial. In many cases, you actually gain more insight than with in-house billing, without needing to manage the day-to-day details.
Q2: Is my data secure with a billing company?
Yes. Reputable billing companies operate under strict HIPAA compliance frameworks and often have more advanced security infrastructure than small-to-mid-sized practices can maintain on their own.
Q3: Is outsourcing billing expensive?
Most billing services charge a percentage of collections rather than a flat fee. This means their incentives are aligned with yours. They earn more when you collect more, making it a performance-driven partnership.
Quick Comparison: Billing Automation vs. Outsourcing
| Factor | Billing Automation | Outsourcing |
| Speed | High | High |
| Expertise | Limited to the in-house team | High (specialists) |
| Cost Structure | Fixed / upfront | % of collections |
| Control | Full | Shared with visibility |
| Scalability | Moderate | High |
The Bigger Picture: Why the Best Practices Use Both
Here’s something the either billing automation vs. outsourcing framing misses: these two approaches aren’t mutually exclusive. In fact, the most efficient practices today are using automation as the operational infrastructure of their billing and outsourcing the strategy and human judgment layer on top of it.
Think of it this way. Automation handles the high-volume, repeatable tasks at speed and scale. Outsourced billing specialists focus their expertise where it matters most, on complex claims, high-value denials, payer relationships, and compliance decisions that require real knowledge and experience.
A practical exampleA multi-specialty group practice uses automated claim scrubbing and eligibility verification to handle their daily volume. Their outsourced billing team then monitors denial patterns, appeals rejected claims, and flags coding opportunities the automated system missed. The result: faster clean claim submission and higher net collections, because neither the software nor the human team is being asked to do something it’s not best suited for. |
This combined model also creates resilience. If payer rules change, your outsourced specialists adapt. If your patient volume spikes, the automation scales. Neither alone provides both of those things.
The practices that struggle most with billing are often the ones that have invested in one without the other, either relying on software they don’t fully use, or outsourcing without any internal systems to support clean data input on the front end. When both elements work in concert, the efficiency gains compound rather than just add up.
How to Think About What’s Right for Your Practice
Rather than prescribing a single answer, here are the honest questions worth sitting with:
- What is your current denial rate?
If it’s above 10%, that’s a signal that something in your billing process needs more than automation can fix on its own. Denial management is a human-intensive task.
- How much staff time goes to billing?
If clinical or administrative staff are being pulled into billing tasks, that’s a hidden cost that often exceeds what outsourcing would actually cost.
- What’s your payer mix complexity?
Practices with complex specialty billing, high Medicare/Medicaid volume, or multiple payer contracts benefit most from specialized human expertise.
- Are you planning to grow?
Growth creates billing complexity. The systems and support structures you set up now will either scale with you or hold you back
Summary
There’s no one-size-fits-all solution for medical billing. What works best depends on your practice’s size, specialty, payer mix, and growth stage. Understanding the strengths and limitations of each approach is the essential first step.
By evaluating your current billing performance, claims, denials, and collections, you can uncover hidden revenue opportunities and identify where improvements will have the biggest impact.
To see exactly how your practice stands, you can book a consultation to review your billing process and explore strategies for maximizing collections and efficiency.